Pain is one of the most common reasons individuals call a rescue. In the rear of a moving lorry, with devices rattling and no warranty of a quick health center handover, the standard you set in those initial mins shapes the client's trajectory. The unit PUAEME008 Offer Discomfort Monitoring furnishes responders to examine, treat, and re‑assess discomfort safely in the pre-hospital context. It mixes clinical judgment with operational discipline. The results are concrete: fewer call for help on scene, smoother extrication, more secure transportation, and improved patient contentment. For numerous clinicians, it additionally functions as a foundation enter wider discomfort administration training courses and certificate pathways that diversify method beyond emergency care.
This guide unpacks the skills, assessments, and results that PUAEME008 anticipates. It links those assumptions to everyday work, and it indicates reasonable training courses, whether you are a paramedic in a country station, a registered nurse moving into occasion medicine, or a physio therapist seeking proficiency in emergency discomfort monitoring for sports insurance coverage. The emphasis stays on what in fact works when time is short and the photo is messy.
What PUAEME008 Covers and Why It Endures
The device sits within public safety and emergency administration training bundles in Australia. Its extent is deliberately sensible: safe, timely, and ethical management of discomfort alleviation in the area. Graduates ought to have the ability to examine pain, select the ideal modality, provide within extent, screen effect, and rise when required. The system supports carriers who might encounter a child with a fractured lower arm at a sporting activities oval, a farmer with a crush injury in a shed, or an older adult with a hip crack on a cool workshops for nurses in pain management restroom floor.
It is not a pharmacology lecture disguised as a proficiency. You will certainly find out analgesic alternatives pertinent to your range, however you invest as much time on patient analysis and environment control as on dosing graphes. The toughest specialists end up being deft at gathering the minimum details needed to act without missing out on red flags. They maintain procedures at their fingertips, yet they customize to the person before them.
PUAEME008 likewise functions as a bridge. Lots of that finish it later pursue a discomfort monitoring certification training course or discomfort management accreditation that broadens to chronic and step-by-step discomfort. Others stitch it into a mosaic of short programs in pain administration and advanced life assistance, creating an account that fits occasion health, mining sites, or retrieval services. Due to the fact that the device lines up with a narrow however important slice of treatment, it maintains its value throughout settings.
Assessing Pain When Time and Space Are Tight
The analysis series is greater than a range. It is an organized conversation, visual scan, and fast physical exam that records both the extent and the pattern.
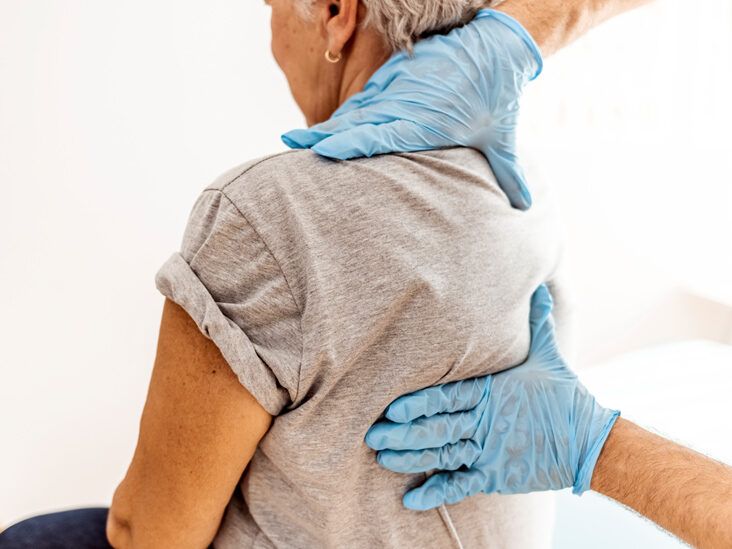
You start with the patient's words. Ask open, after that concentrated concerns: Where is the pain, what does it feel like, when did it begin, what makes it worse or far better? If you are making use of a numerical score scale, established context. I will certainly ask you to rank your discomfort from zero to ten, where zero is no discomfort and ten is the worst you can think of. Also knowledgeable medical professionals miss this sentence, and people respond with a number that does not match their interior yardstick. In kids, usage encounters scales or easy descriptors. In nonverbal adults, sew together breathing pattern, articulation, face stress, muscular tissue protecting, and essential indicator trend.
You associate the tale with visuals and palpation when proper. Look for crookedness, deformity, strained compartments, pallor, cyanosis, and swelling that breakthroughs during your time on scene. Move joints proximally and distally only if it does not intensify harm. Think about a second survey when the device suggests concealed injuries. I as soon as dealt with a client who focused on shallow lower arm pain after a fall, only for a fast hips rock and leg-length check to disclose a more severe hip injury. The pain they report is not constantly the pain that will certainly eliminate them.
Vital indicators matter, yet they can deceive. Hypertension and tachycardia can show discomfort, worry, or hypoxia. Alternatively, a well-conditioned athlete may reveal marginal change regardless of extreme pain. Informed pattern recognition assists: a groaning individual with a rigid abdomen and a heart rate climbing from 90 to 110 often needs quick transport and mindful analgesia, not prolonged probing.
Consciousness and cognition belong to the assessment. A head-injured patient who can not track an easy conversation can not reliably self-report. Readjust your evaluation strategy and recruit a caretaker, however avoid letting 3rd parties overwrite the patient's very own assumption if the client has the ability to communicate.
Pharmacological Options Within Scope
The unit recognizes that extents vary. A basic -responder may have dental or inhaled options; sophisticated service providers may carry IV or IO representatives. The task is not to remember every medication on the market, but to grasp secure use of those you carry.
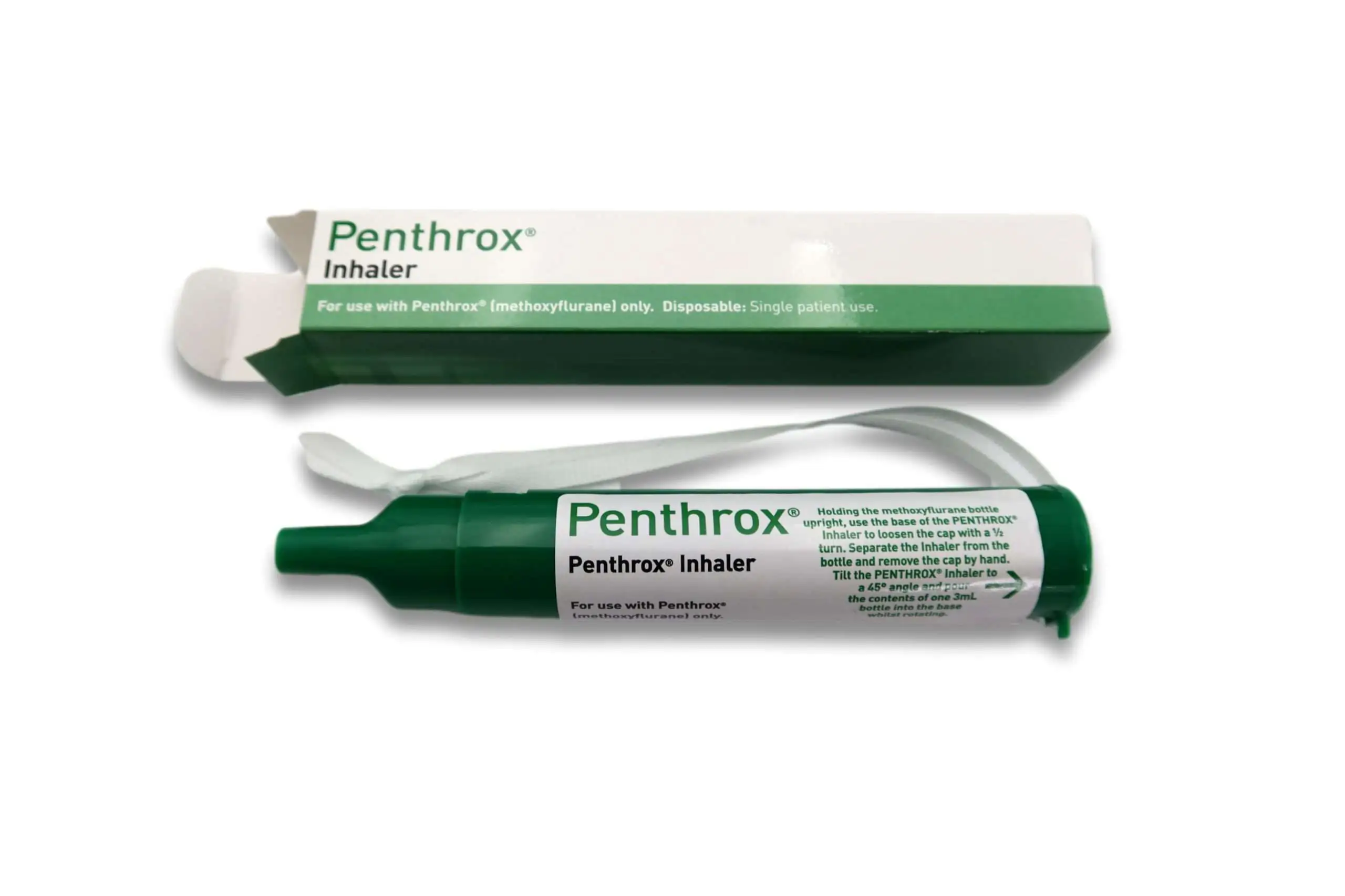
- Methoxyflurane: A staple in numerous pre-hospital kits for moderate to severe pain, especially bone and joint injuries. Quick beginning, non-invasive, and patient-controlled inhalation. Secret training factors include stopping too much exposure throughout extended usage, ensuring adequate ventilation in restricted spaces, and staying clear of use where malignant hyperthermia risk or significant kidney disability is suspected. For anxious people, the act of holding the inhaler adds a sense of control that frequently eases the total distress curve. Oral analgesics: Paracetamol and NSAIDs stay workhorses for light to moderate discomfort if the patient can ingest and has no contraindications. Splinting plus oral analgesia can decrease transportation pain for easy fractures. Watch for timing, cumulative dose with patient's self-medication, and NSAID warns in renal condition, peptic ulcer, and bleeding risk. Nitrous oxide/oxygen mix: Useful for procedural discomfort like manipulation or extrication. It calls for devices checks, appropriate scavenging, and attention to clients with pneumothorax or digestive tract obstruction where gas development provides hazards. The short half-life permits quick review after the procedure. Opioids: Morphine and fentanyl are common at innovative degrees. They continue to be efficient for serious pain when titrated to result, particularly in injury. The pre-hospital context raises the importance of air passage alertness, collective sedation with alcohol or benzodiazepines, and step-by-step dosing with clear endpoints. Fentanyl's hemodynamic stability often makes it a favored selection in hypotensive trauma. In older grownups, start with smaller sized increments and extend your review periods a touch longer. Ketamine: In sophisticated procedures, low-dose ketamine provides strong analgesia with minimal breathing anxiety. It beams in hypovolemia, burns, and trapped patients. Emergence phenomena are unusual at analgesic dosages yet can be minimized with silent training and, if extent allows, a tiny benzodiazepine accessory. Prevent the lure to rush the dose; a sluggish press over numerous mins smooths the ride.
The heart of PUAEME008 is security. Whatever agent you choose, validate five legal rights, look for allergic reactions and considerable comorbidities, file batch numbers where called for, and display oxygenation, air flow, perfusion, and psychological standing. Never ever let a syringe lock your attention more than the individual's upper body surge and fall.
Non-Pharmacological Actions That Outperform Their Reputation
An unusual quantity of discomfort yields to fundamental measures that need no prescription. Rigid splinting for long-bone fractures, sling and swathe for shoulder injuries, mild grip and alignment within extent, and cushioning bony prestiges all count. With burns, very early cooling with cool, not cool, water for up to twenty mins improves pain and results, but do not postpone transportation for prolonged cooling on deep or considerable burns.
Positioning remains a powerful device. People with stomach discomfort typically prefer knees bent. Chest discomfort patients usually choose a semi-Fowler setting that relieves lack of breath. Regard their selected stance unless it disputes with various other priorities like back protection.
Psychological support changes physiology. Talk in constant tones, established expectations, and tell your activities. On a country road after a rollover, I invested two mins describing precisely what the splint would certainly seem like as I applied it. The individual's breathing rate reduced from 28 to 20 before we touched the arm or leg. PUAEME008 treats such interaction as an expertise, not a soft add-on.

Cold and warmth treatments depend upon the injury. Ice reduces swelling and discomfort in intense sprains and pressures, ideally covered to stay clear of skin injury. Warmth can assist muscle mass spasm, but prevent it in acute trauma or where swelling is developing.
Special Populations, Subtle Differences
Children interpret discomfort via household cues and atmosphere. A moms and dad's face will certainly matter more than your uniform. Come down to eye degree, reveal the mask or inhaler initially, and allow them touch non-threatening tools. Dosage medications on weight, not age, and validate numbers with caregivers and your referral. Step-by-step discomfort climbs considerably in kids, so plan analgesia before cannulation or fracture control. Take into consideration that dehydration increases medicine effects and negative effects. Reassess usually and record behavior, not simply numbers.
Older adults provide a different difficulty. They might under-report discomfort or normalize it. Polypharmacy and comorbidities boost risk. Examine for delirium and cognitive disability. Avoid opioid piling with existing sedatives, and titrate gradually. For hip cracks, mild alignment and grip, plus a heat pack to the lumbar region for muscle mass leisure, can save an opioid dose or 2. In the presence of renal illness, be judicious with NSAIDs.
Pregnancy makes complex pharmacology and positioning. Lateral tilt beyond mid-second trimester safeguards venous return. Several services prefer fentanyl or low-dose morphine over NSAIDs in late pregnancy. Stomach pain in pregnancy is entitled to a reduced limit for transport and consultation.
Patients with substance use conditions deserve the same roughness as any individual. Prevent stigmatizing language. Titrate to impact, document fairly, and keep security through positioning and monitoring. Mixed drunkenness with alcohol can mask hypoventilation, so set a high bar for pulse oximetry and capnography where available.
Scene Administration and Crew Coordination
Emergency pain management does not take place in a vacuum. The unit anticipates you to incorporate analgesia with scene security and logistics. If extrication is pending, plan your analgesic home window so discomfort relief peaks during activity. On a steep driveway with a fragile shoulder misplacement, we changed timing so methoxyflurane gotten to effect right as the client transitioned to the inside story stretcher.
Agree on duties. One medical professional manages the air passage and keeps an eye on sedation degree. The other communicates dosing out loud and documents. Closed-loop communication stops double dosing, especially when syringe swaps take place under stress. Alert getting facilities to drugs given, timing, and effect so they can improve your strategy instead of repeat or reverse it.
Equipment checks are not busywork. A missing out on mouth piece, a vacant nitrous cyndrical tube, or a dead suction battery can hinder great objectives. Several staffs utilize brief responsive checks at change beginning: turn the valve, feel the flow, click the capnography cable television, press the bag. Discomfort monitoring training courses typically build these routines into simulation circumstances to make them automatic.
Documentation that Informs the Story
A crisp narrative supports client security and lawful protection. Graph preliminary discomfort descriptors, scale ranking, and location. Compose what you provided, just how much, when, and why you chose it. Include non-pharmacological actions, client placing, and splinting technique. Reassessments must read like a timeline: 14:12 fentanyl 25 mcg IV, 14:16 discomfort 8 to 6, RR 18, SpO2 98 percent on 2 L. Stand up to the urge to document only numbers. Behavior, face, and feature provide richer detail. Person able to birth weight with assistance at 14:29 carries even more meaning than a lone score.
When discomfort stays refractory, note what you dismissed and your acceleration actions. If you consulted medical control or elderly medical professionals, list their advice. In multi-agency occasions, share a summary with on-scene managers to stay clear of treatment gaps.
Training Pathways: From Unit Proficiency to Certification
Many suppliers start with PUAEME008 as a targeted stepping rock. It gives a functional toolkit you can utilize the following shift. From there, individuals diverge based on duty and interest.
- Pain administration training for registered nurses: Nurses in immediate care, perioperative settings, or remote centers often add innovative evaluation, procedural analgesia, and titration protocols. Pain management training courses for registered nurses in some cases include modules on multimodal therapy and opioid stewardship customized to nursing scope. Certificate programs may stack PUAEME008 with wound treatment, IV therapy, and sedation competencies. Pain management programs for physio therapists: Physios that cover sports events or work alongside emergency groups gain from sharp pain structures, splinting, and non-pharmacological approaches. These pain monitoring training programs value the physical rehabilitation scope while educating clear referral sets off. Combination with blast and spinal evaluation modules is common. Provide pain management training course for pre-hospital experts: Ambulance solutions and event medication providers run short training courses suffering monitoring, commonly lined up to PUAEME008 supply pain management. They concentrate on inhaled agents, nitrous, and opioid titration with rigorous air passage tracking. The much better programs consist of nighttime and cramped-space simulations. Pain administration certification and qualification pathways: If you want to broaden beyond severe care, seek a certificate program suffering management that addresses severe, chronic, and cancer discomfort. A pain administration certification program normally covers neurobiology, psychology of pain, useful analysis, and pharmacology across the continuum, plus communication skills and moral considerations. Some programs identify prior picking up from PUAEME008 and reduce your path.
Not all pain administration courses are equal. Review training course hours, professors experience, simulation realism, and post-course assistance. Ask whether situations reflect your practice setting. I favor programs that consist of failed-response situations and gray-zone decisions, not simply textbook fractures.
The Ability of Titration and the Art of Timing
Titration divides confident providers from hesitant ones. The objective is not lack of pain, however appropriate discomfort that maintains security and function. For numerous trauma patients, relocating from a 9 to a 4 or 5 allows you splint and transport without fogging the respiratory tract. That balance takes dosages in small actions and stops for effect. Fentanyl peaks quickly, ketamine a little bit slower at analgesic doses, and oral agents lag by 10s of minutes. Your plan needs to value these pharmacokinetics.
Timing issues as high as the complete dosage. If you will certainly bring a patient down three flights, peak result should get to the landing, not at the aesthetic. For procedural steps like shoulder reduction, pick either fast titration of a short-acting representative or a ketamine analgesic dosage with quiet coaching, depending on scope and ability mix.
Beware dose momentum. After 2 small doses yield only little gains, groups frequently leap to a huge 3rd dose that overshoots. Persistence and review stop see-sawing between discomfort and oversedation. Usage capnography where possible. A subtle higher creep in ETCO2 may be your first warning.
Ethical Grounding: Permission, Equity, and Opioid Stewardship
PUAEME008 expects you to get grant the degree possible, even under stress. Explain advantages and dangers in ordinary language. A straightforward manuscript works: I can offer you a medication with your blood vessel that need to decrease your discomfort in a few mins. It can make you drowsy and slow-moving your breathing a little bit, so I will certainly enjoy you closely. Is that alright? For inhaled representatives, demonstrate and let the person hold the tool when appropriate.
Equity issues. Individuals from marginalized groups typically report obtaining less analgesia for the exact same injuries. Build a habit of structured evaluation and documentation to counter implied prejudice. If your numbers and narrative justify therapy, follow through irrespective of accent, age, or regarded stoicism.
Opioid stewardship in the pre-hospital space depends upon titration, surveillance, and handover quality, not on withholding required analgesia. Your function is to alleviate intense suffering safely, not to establish long-lasting opioid trajectories. Clear documentation and communication support the receiving group in preparing following actions, including non-opioid methods and discouraging when appropriate.
Measuring Outcomes That Matter
The simplest pen is the pain rating pattern before and after therapy, however outcomes surpass a number. Watch for boosted tolerance of required motion, minimized stress and anxiety, secure vitals, and the lack of damaging events. In solution audits, meaningful end results consist of the portion of qualified injury patients that got prompt analgesia, typical time to initial dosage, and the rate of considerable respiratory depression per 1,000 administrations. Lots of solutions additionally track patient-reported experience procedures at follow-up. Comments like They informed me what to anticipate and I felt cared for frequently associate with better physical trajectories.
For private experts, maintain an individual log. Note what worked, what really did not, and why. Patterns arise: dosing that is regularly sluggish, skills that require refresher courses, or methods that could utilize clarification. Bring these monitorings to training leads. Good discomfort monitoring training adapts based upon frontline feedback.
Common Mistakes and Practical Fixes
Two errors repeat. The first is dealing with the number, not the individual. A teenager who ranks discomfort at 10 however giggles with close friends could be using the range differently or coping well. Concentrate on feature and behavior as well. Can they move with assistance, or do they tense and guard at every motion?
The second is avoiding the review. After the first wave of analgesia, re-examine the injured location et cetera of the body. Swelling may have advanced. A limited splint might require loosening. That five-minute check protects against complications and tweaks dosing.
Other side cases should have attention. In thermal burns, stay clear of hefty dosages that cloud airway evaluation. For abdominal pain where surgical procedure is likely, modern-day evidence sustains suitable analgesia rather than the old anxiety of masking indicators. Still, maintain doctors in mind and record searchings for clearly before and after therapy. In suspected compartment syndrome, pain disproportionate and pain on passive stretch persist regardless of analgesia. Escalate early.
Building Skills Via Deliberate Practice
Competency increases with rep, however arbitrary repeating is slow-moving. Calculated method presses learning time. Create micro-drills. Prior to each shift, verbalize your methoxyflurane contraindications while you set the package. When you replenish fentanyl, practice a three-step titration plan for a 70 kg adult and a 40 kg older adult. Pair with a colleague and review each other's consent scripts.
Simulation ought to feel like work. Dim the lights, include noise, and imitate the ache in your shoulder as you kneel by a child seat. Run series where the client does not respond to your initial strategy so you practice acceleration without panic. Use a metronome for slow ketamine pushes to avoid the too-fast hand that invites side effects.
Finally, purchase wider learning. A pain management certificate or an organized pain administration program subjects you to the biopsychosocial design and multimodal approaches. Physiotherapists will certainly deepen non-pharmacological methods. Registered nurses will certainly refine titration in step-by-step settings. Pre-hospital companies will certainly harmonize sedation scales with transport truths. The most effective programs treat PUAEME008 as a support point and build external with nuance.
The Reward: Calmer Scenes, Much Safer Transports, Better Trust
The very first time you minimize a patient's 9 out of 10 to a manageable 4 as you fill them, you really feel the space adjustment. Households take a breath. Crew participants stop seeing the clock and start assuming two continue. The person keeps in mind that experience in different ways, and they are more likely to involve with treatment on arrival. Across thousands of instances, this equates right into less combative transports, less failed procedures, and less damaging events.
PUAEME008 Supply Discomfort Monitoring instructs not only how to push a medicine or apply a splint, but just how to orchestrate the small choices that make acute discomfort acceptable without compromising security. It prepares you for the confined spaces and imperfect information that define pre-hospital job. Combine it with proceeded pain monitoring training, look for feedback, and maintain refining. The ability deserves the effort, and the end results show on every shift.